Impaired Liver And Hormones
Impaired Liver
The liver is an energy reservoir. It’s the main communication channel that tells the thyroid to produce hormones keeping the body in check. If the liver is impaired or stressed through various inputs (e.g. stress, poor diet, lack of sleep, etc.), the thyroid cannot receive the proper instructions for normalizing hormonal activity.
What ends up happening with a scrambled communication signal between the liver and the thyroid is an accumulation of anti-hair growth hormones as a result of thyroid disruptiveness. When both these important organs shut out, what is known as “The Hair Loss Avalanche” (all the events at the intercellular level leading up to hair loss) is at its greatest!
One of the early signs of hormonal imbalance due to an unhealthy liver is a change in the testosterone:estrogen ratio. The ratio is different for male and female victims of hair loss, so make sure you read the applicable following sections carefully.
Estrogen: Testosterone Dominance
Men
For men, too much ESTROGEN, specifically estradiol (also known as E2 or 17β-estradiol), with too little testosterone elevates prolactin, which is bad for the hair. In this study[1], 65 males with androgenetic hair loss had elevated E2.
Furthermore, this mice study[2] solidifies the catastrophic effect of topical 17β-estradiol on the hair cycle. To save you time, I went ahead and laid out the three key findings:
- Prolongs the catagen (regression) while sustaining the telogen (resting) hair phases
- TGF-β2, a hair antagonist (bad), is upregulated in the dermal papillae causing the hairs to be stuck in catagen
- BMP-4, a hair antagonist (bad), immediately increased after catagen further sustaining telogen and preventing a transition to anagen
The good news is the stem cells were still intact and alive in the dermal papillae and weren’t affected by application of 17β-estradiol. What that basically means is once estradiol was back to normal or no longer applied, because the stem cells are still present, dormant hairs have the capability of coming back to life. So long as the stem cells are alive, they are active, and can reproduce lifeless hairs.
To further shed estrogen’s carnage, it’s “venomous” behavior on hair growth were even notated as far back as 1958, in The Biology of Hair Growth.[3]
Don’t be fooled though, because there’s another side of the coin. A high estrogen:testosterone ratio is only one standard to consider if you’re a male losing your hair. It turns out, male pattern baldness can also arise from a high testosterone:estrogen ratio meaning testosterone is more prevalent than estrogen as this study[4] indicates.
Women
On the contrary, women who have too little estrogen and too much TESTOSTERONE can experience the similar hormonal temperament as men as explained by Dr. Eric Berg.[5]
Dr. Berg’s explanation is further expounded by Yelva Lynfield’s experiment with pregnant females. She noticed during pregnancy, when estrogen is at its near high, anagen hairs increased profoundly. At postpartum period (delivery), hair loss soared when estrogen plummeted.[6]
And in this study[7], 20 premenopausal women with pattern hair loss had a lower estradiol:free testosterone ratio.
A healthy liver produces PROGESTERONE, which deactivates estrogens and protects testosterone from converting to DHT. Low progesterone is indicative of hair loss due to more DHT conversion. This is one main reason why postpartum women sometimes lose their hair because progesterone tends to fall steeply.
Then again, female pattern hair loss can also happen in the other direction if there’s too much estrogen and too little testosterone. In vitro (test tube), using female occipital hair follicles and 17-β-estradiol (E2), this study[8] confirms significant inhibition to hair shaft elongation. And in this article[9], estrogen DOMINANCE causes hair loss in women due to thyroid inhibition.
Take Home Message
- Unfortunately, there isn’t a gold standard to use, otherwise, hair loss would no longer be pervasive. The best indicator is to watch out for any hormonal DOMINANCE on either side of the estrogen:testosterone scale.
- Like men, the hormonal ratio must be well balanced on both ends. If any one hormone is more DOMINANT than the other, exhaust all options to reach equilibrium.
- Order a blood test for estrogen, free testosterone, and total testosterone to monitor any imbalanced shifts.
Sex-Hormone Binding Globulin (SHBG)
Another hormone disturbed by an unhealthy liver is SHBG. An SHBG paucity can lead to diffuse hair loss in some women.[10] It may also contribute to premature androgenetic alopecia (AGA) in men.[11] The theory is by having more SHBG, free testosterone is no longer unbound making it less likely for DHT conversion via 5-alpha reductase.
There are some formidable “forces” one should look out for to keep SHBG stable. If taken lightly, DHT is more likely to invade the hair follicles effortlessly. I’ve labeled them below:
- Less SHBG = high insulin resistance and glucose in the blood[12] (to read more about insulin, click here for a prologue)
- Less SHBG = high blood pressure[13] (hypertension)
- Less SHBG = obesity[14]
- Less SHBG = higher smaller, denser low density lipoprotein (LDL) or bad cholesterol and increased triglyceride[15]
Cortisol: Stress Bomb #1
One of the big stress hormones secreted by your adrenal glands is CORTISOL. Cortisol typically rises in the morning after you get out of bed to prepare you for the day. It then drops in the early afternoon and levels throughout the entire day, unless if there are other stressful inputs (job deadlines to satisfy, relationship problems, etc.). The body releases cortisol during distress (bad stress), when anxiety or fear kicks in as a fight-or-flight mechanism. It can also be produced during eustress (healthy stress), such as when you’re motivated to fulfill a goal.
The type cortisol you should be concerned about is when the body enters into consternation in the form of DISTRESS. When this happens, especially in a repetitious cycle, mitochondrial cellular activity shuts down. In case you’re unaware, mitochondria is the power line that supplies “electricity” to all our cells. If the mitochondria is impaired through continuous stress, it’s unlikely any treatment will have a profound positive effect on hair loss or any other ailment.
Stress can also come in a subtlety, which is overlooked by society. That subtlety is sleep deprivation. Our bodies were made to rest. Even God rested on the seventh day. On average, although age may be a factor, 7-8 hours of sleep per day is the ideal standard to aim for. Chronic, sustained sleep loss, if not taken seriously, ascends cortisol. Even partially losing 3 hours of sleep can radically spike cortisol on the second evening day following the night of sleep.[16] This study[17] further validates the aforementioned finding.
Sleeping less than 7 hours or even 9-10 hours also opens the door for another health “bully” – DIABETES. In a population of 744 participants, the sleep deprivers (< 7 hours of sleep) and the sleep overachievers (9-10 hours of sleep) were directly associated with type 2 diabetes due to higher insulin resistance.[18] Note, if you want to know how INSULIN RESISTANCE is connected to hair loss, click here.
In relation to hair loss, the constant, accrued flow of cortisol blocks TSH from making free (unbound) T4 and T3 from the thyroid to regulate metabolism. T3 is critical for inducing mitochondria. If the thyroid is held “hostage” from the “most wanted public enemy”- CORTISOL– and instead, produces reverse T3, which is inactive, how will you regrow your hair if the mitochondria is suppressed?
TSH is a signal from the pituitary gland to make T4 and doesn’t do anything until it’s converted to T3, which promotes mitochondria and hair growth. If you’re stressed out, you won’t make T4, but instead reverse T3.
Proper mitochondrial signaling using thyroid hormones is vital for instructing the pool of stem cells located in the hair bulge to move and proliferate new hair. When there’s too much cortisol, the liver discharges Thyroid Binding Globulin (TBG). This protein is detrimental because it binds free T4 and T3 in circulation.
When free thyroid hormones are bound, they are inactive. If T3 is no longer free, the cells lose mitochondrial function, progesterone drops, and estrogen elevates. At this point of estrogen dominance, it has been shown TBG directly intensifies[19] creating a perfidious feedback loop, which impairs T3’s liberty.
Because cortisol is “dynamite” to the thyroid, there’s no surprise why balding men and women have immoderate concentrations of cortisol.[20]
Prolactin: Stress Bomb #2
PROLACTIN is a hormone secreted by the pituitary gland to stimulate milk production during pregnancy. It’s also produced during physical or emotional stress, similar to cortisol. Too much of it “freezes” the hair follicles in the catagen phase (regression) thereby significantly reducing its size.[21] To further add more color, it may so happen be prolactin only significantly slows anagen entry if it’s abundant and sustained over a long period as demonstrated in this mice study.[22] Temporary prolactin spikes or moderate prolactin levels most likely unalters the hair regrowth cycle unfavorably.
Prolactin also shares a direct affiliation with estrogen and many other molecules, such as prokinetics, opiates, anti-androgens, anti-hypertensive drugs, etc.[23] Until research proves otherwise, estrogen stands out among the list of prolactin-inducers when we think in terms of hair follicle regulation. Estrogen is a prolactin stimuli.[23] If estrogen increases, so will prolactin.[24]
This paper[25] actually does a good job tying the direct connection of estrogen’s, cortisol’s, and prolactin’s response to AGA. All three “silent hair assassin” hormones were elevated in the study, which confirms the strong behavioral correlation they share with each other (e.g. if estrogen increases, that response may very well cause a rise in cortisol and prolactin).
We all know excess estrogen, scarce progesterone, and mitochondrial degradation are one of the major culprits behind a volatile thyroid and with that comes hair deterioration.
Insulin Resistance Morphs Into Powerful Androgens
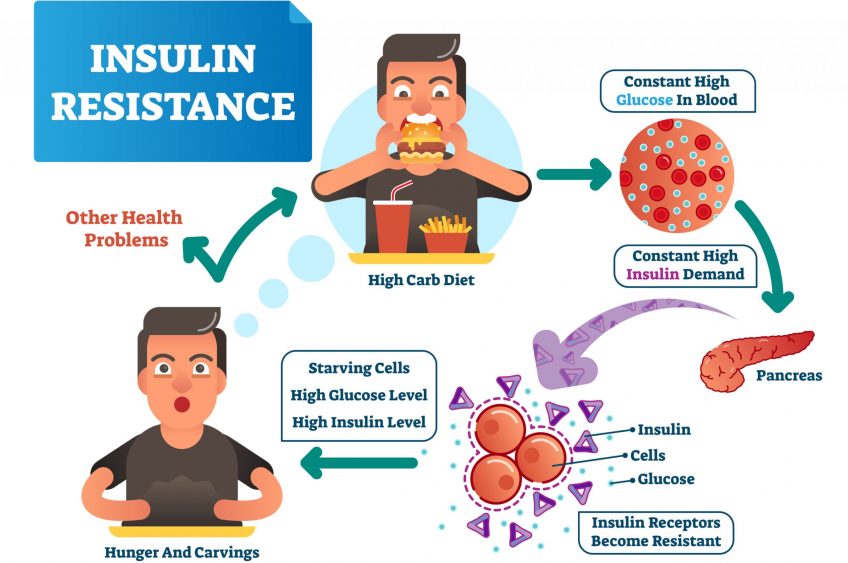
Blood sugar control is integral for hair and health survival. Your pancreas manufactures a hormone called insulin. Insulin responds to sugar or any food (refined carbs) that turn into sugar. Its primary job is to reduce sugar in your blood. If you’re hypoglycemic – having abnormally low levels of sugar (glucose) in the blood – the receptors on your cells don’t respond to insulin.
Over time, if insulin cannot enter the cells because the body is not allowing it in a hypoglycemic state, insulin piles up on massive proportions. This can potentially happen if you’re consuming the wrong types of foods mainly a high, refined carbohydrate or sugar diet, which promote excessive fat stored on the liver and pancreas. Lack of sleep and physical inactivity are also common causes.
If the cells are resistant to insulin, sugar will accumulate in the blood over a period of time because insulin cannot enter into the cells to lower the sugar. This is known as INSULIN RESISTANCE, which eventually speeds the onset of DIABETES!
If you’re want a more in-depth explanation on insulin resistance, watch Dr. Eric Berg’s video.[26]
When diabetes comes into play as a result of prolonged insulin resistance, chronic inflammation, and obesity are not only calls for action. What also ends up happening is excessive insulin and glucose in the blood translates into more androgens and less SHBG.[27] For women and men with less SHBG that can mean more free, unbound testosterone is available to convert into DHT. With more DHT floating around your body, depending on your androgen receptors’ sensitivity, the risk of developing AGA can tremendously increase in some, not all cases.
And if that’s still unconvincing, here are three studies cementing the commonality of insulin resistance in AGA:
- Study #1[28] – also identified diabetes, a derivative of insulin resistance, and high blood pressure (hypertension) in patients with AGA.
- Study #2[29] – concluded higher insulin resistance in AGA patients emulating polycystic ovary syndrome in women.
- Study #3[30] – found significant levels of insulin resistance, free testosterone, and lipids in young males with a Norwood type III hair loss.
Take Home Message
- Too much or too little sleep elevates cortisol
- Cortisol suppresses thyroid regulation, metabolism, and hence hair growth by blocking the mitochondria and unleashing TBG.
- To miniaturize the production of cortisol, aim for 7-8 hours of sleep daily, exercise, meditate, and eat nutritious, unprocessed, anti-inflammatory foods.
- Excessive prolactin is a stimuli for shutting out the growth of hair follicles.
- Temporary prolactin elevations will probably not block the normal hair cycle.
- Estrogen shares a three pronged relationship with cortisol and prolactin. If estrogen rises, so will cortisol and prolactin.
- Artificial, refined carbohydrates and sugar, over time can lead to insulin resistance by blocking the receptors on your cells for insulin to enter into.
- Insulin resistance speeds the progression of diabetes and androgens and decelerates SHBG.
- With too little SHBG, more testosterone becomes freer increasing the bioavailability of DHT.
Serum IGF-1: A Hair Loss Master In Disguise
Serum (blood) IGF-1 (Insulin Growth Factor) (not scalp tissue) is a growth hormone developed by the liver subsequently when the pituitary gland releases the growth hormone in the blood. It shares a “yinyang” relationship with insulin that gets repleted from the pancreas. That “yinyang” is symbolic of insulin and serum IGF-1 working in unison to determine which type of fuel to use – sugar (insulin) or fat (IGF-1).
The decision rests on whether you consume foods or fast. Eating will cause the pancreas to secrete insulin, thus using sugar. On the contrary, fasting exudes more serum IGF-1, which means more stored fat is recycled as fuel.
Ever noticed why intermittent fasting in the short term is effective for losing weight? Well it’s because serum IGF-1 kicks in as a good side effect from and burns off excess stored fat through fuel consumption. There are other methods of increasing serum IGF-1 like adhering to protein intake, capacious sleep, dairy, grains, and strenuosity.
Due to serum IGF-1 being four to five times more potent than insulin[31] and how various commodities can quickly increase its bodily presence, serum IGF-1 is a highly sensitive wire that can trigger an explosion. The explosion I am referring to is pattern hair loss originating from a hormonal disorder.
Before I get into the serum IGF-1 drama, an important distinction needs to be made between free/unbound and bound serum IGF-1.
Free And Bound Serum IGF-1
What holds more weight when we speak about serum IGF-1 in the context of hair loss is the amount of free vs. bound serum IGF-1. As you will see, research points in the direction that baldness may be caused by elevated free serum IGF-1 and lower insulin-like growth factor binding protein 3 (IGFBP-3). Although that answer is not definitive due to a deficit of follow up studies, the current reports are still present and strong enough to accept this argument. Just like there are current studies validating less SHBG (the binding testosterone hormone) and more free testosterone in bald subjects, it’s in a very similar reason to believe more unbound/free serum IGF-1 can attenuate hair growth.
IGFBP is comprised of a family of six binding proteins. About 98 percent of serum IGF-1 is almost always bound to one of the six binding proteins. I say almost always because if serum IGF-1 is highly elevated, there’s strong reason to believe in respect to the vertex balding study[32], a pronounced presence of free serum IGF-1. If there wasn’t, then those vertex balding subjects would probably have more hair if free serum IGF-1 was bounded to one of the IGFBP family proteins, the most abundant being IGFBP-3.
Note, in that same study, IGFBP-3 was scarce. This type of binding protein is amplified in human dermal papilla hair cells along with IGFBP-5.[33] It also modulates tissue IGF-1 through the production of keratinocytes in the epidermis[34], which play a role in hair follicle formation. And the fact IGFBP-3 influences cellular hair proliferation[35] goes to show it has a significant spotlight in the hair cycle.
Much emphasis should be placed on IGFBP-3 for future hair loss studies given it makes up 80 percent of all IGF binding proteins.[36]
Is All Serum IGF-1 Bad?
Modest to moderate amounts of serum IGF-1 is not a bad thing. We actually need enough serum IGF-1 for cellular proliferation ranging from muscular and bone growth to brain development to cardiovascular healthiness. It’s when we have a surfeit where danger is at close waters. Unfortunately, because of my ignorance, I became that victim of overloading on serum IGF-1 through WHEY PROTEIN SHAKES, which costed me most of my hair.
Before we take an excursion to my ominous whey protein story, allow me to quickly switch gears to the relevance of TISSUE IGF-1. Tissue IGF-1 is not the same as serum IGF-1. The former actually regrows hair by attaching to the IGF-1 receptors on the scalp thereby regulating the hair cycle. As indicated in this mice study, exogenous application actually prolonged the anagen phase and regrew hair on bald mice.[37] It’s a potential strong hormone to accelerate hair growth that Japan’s famous director, Dr. Kenji Okajima, and his research team have founded an IGF-1 treatment clinic.[38] Tissue IGF-1 is also induced in the scalp by wounding (e.g. dermarolling) or other mechanical stress techniques (e.g. massaging or bristle boar brushing).
So, the big takeaway is serum IGF-1 only in prodigious amounts is deadly to the hair whereas tissue IGF-1 is pro-hair.
Circling back to my horrific whey protein story, at age 22 I was taking a ridiculous amount of four scoops per day five days a week to gain muscle mass. To give you some perspective on how many daily grams of protein that was exclusive from my normal dietary meals, 96 grams was the lucky number!
Now, take that number and add it with the 60 or so grams of protein I got from my inflammatory diet each day. And it doesn’t end there! Add on weight lifting plus cardio exercises four days a week along with 8-9 hours of sleep per day for a two year time span. Can you guess what kind of impact my rigorous regimen had on my liver? A constant, colossal overflow of serum IGF-1. And because my liver couldn’t handle all the protein, especially the artificial whey kind, more insulin was also unleashed according to Dr. Berg.[39]
I think the science will be a lot clearer if I rewind and take a snapshot of my observations in the past to see how they line up with the medical literature.
Observation #1: Modified Western Diet Supports Pro-Inflammation
Regular intake of inflammatory, refined carbohydrate, and refined sugary foods (grains, polyunsaturated fats, etc.) raised my insulin to lower the high glucose from these high glycemic foods. My liver also produced more free/bioavailable (unbound) serum IGF-1 in response to this high glycemic load diet.
As indicated in this study, it’s known a Western diet both increases insulin and IGF-1, which overtime, can lead to other complications like type 2 diabetes and cancer.[40] Hyperestrogenemia (excess estrogen) is also heavily influenced by such a diet[41] shifting the estrogen:testosterone ratio to one that’s more estrogen dominant. With more insulin, estrogen, and free serum IGF-1 cruising in my blood stream, my body and hair were in for a big, grisly surprise.
Probably, the only good aspect about my Western diet was that it was modified to the extent of eating organic meats (cold cuts, chicken, and turkey), milk, some grains (white rice), and wild caught seafood. If we were to extrapolate the most nutrient-dense foods, chicken, turkey, and seafood would be the winners.
Even though, I was eating a modified Western diet, my diet was still not pristine. I ate other low-quality foods particularly cold cuts, dairy, and whey protein. Despite cold cuts and milk being organic, their biological content still made them risky in terms of insulin-dependency as these medical studies point out:
- Processed meats increases the risk of type 2 diabetes, a symptom of insulin resistance6[42]
- Milk and fermented dairy like whey protein are higher insulinemic foods[40]
- Milk consumption based on 3 servings raises free serum IGF-1 by 18.6 percent[43]
When it comes to whey protein shakes, it was a beast of its own as my next observation reveals.
Observation #2: Whey Protein Shakes Screwed Up My Hormones And Hair

I am doubly and highly convinced my overdose on whey protein shakes was the deal breaker for ruining my health and hair. Here are a mixture of eight plausible theories, observations, and factual evidence proving why I am against whey protein/high-protein diets and how it directly lead to my pattern baldness:

Observation Based On Abnormal Feelings
I’ve always ate the Western diet since inception way before I started taking whey protein. At that time, my hair and health felt great. I was growing hair as fast as a horse and didn’t feel any less different until whey protein came into the picture. Remember, I was taking a hefty load for two years before I started noticing adverse changes to my libido, hair thickness, and gut tolerance.
Don’t get me wrong. Increased libido is a good sign your hormones are working as intended. Mine, though, was extremely inhumane. I was having constant, uncontrollable, sexual, and impure thoughts of women on a daily basis for an extended time. If there was a diagnosis for this disorder, I would probably be classified as OCLD (Obsessive-Compulsive Lustful Disorder). You might be saying, “Joe, that’s normal as a guy in his early 20s”. Maybe, if one cannot control their lustful desires, but I was a different breed. I made a covenant with God through confession not to cognitively dwell on this mortal sin ever. That’s exactly what I did for four long years until whey protein made me feel like an animal all over again. Having such thoughts is one thing if they’re temporary. Having these thoughts and feelings like an animal is another in respect to abnormality.
In addition to my constant aroused feelings, the protein shakes made me feel very bloated and at times, constipated. The casein (protein in dairy) was most likely the cause of my intolerance. I also noticed my hair was beginning to lose its texture and luster once I turned 24. The good news was as soon as I stopped the protein shakes after two years, my sexual arousals were back to normal as I no longer experienced animal-like thoughts and feelings toward women. My bloating also went away. But the horrible news was my hair continued to fall out, only this time at lightning speed.

Dr. Eric Berg's Theory On High-Protein Diets
As I noticed these troubling signs, I knew something wasn’t right. I didn’t exactly know the answer until five years later after I stopped using whey protein. I was able to connect the dots of attributing higher whey protein with higher incidences of free serum IGF-1, when I bumped into Dr. Berg’s insightful presentation titled, “The Underlying Root Cause(s) of Your Hair Loss”.[44]
In that video he confirms soy protein isolates or specific high protein diets can aggravate the liver disconnecting the conversion of thyroid hormones and raising serum IGF-1 causing a buildup of androgens. The serum IGF-1 he was probably referring to was the unbound type, since it’s more bioavailable or freer to bind to androgen receptors, thus potentiating androgenic production.

Ali Kuoppala Scientific-Based Conclusion On High-Protein Diets
It’s no wonder why I was transformed into somebody I wasn’t at the time I became best friends with whey protein. Not only was I making excessive free serum IGF-1 and insulin, but according to Kuoppala, my cortisol skyrocketed putting my health in a shock of exhilarating stress. To add on the misery, my estrogen:testosterone ratio was out of whack probably because of a hormonal imbalance with estrogen being more superior than testosterone.

High IGF-1 Levels In Respect To Whey Protein Supplementation
This study conducted over a period of two years further proves whey protein supplementation significantly elevates serum IGF-1.[46] When I tied this study as well as the four below back to Dr. Berg’s linkage between high serum IGF-1 and high-protein diets, I was factually sold on his theory.

Another Scientific Study Cementing Loose Ends

Vertex Balding Males Had Higher Serum IGF-1 Content Than IGFBP-3

Vertex Baldness Doubled With Men Having Higher Levels Of Serum IGF-1 And Testosterone

Hypoglycemia (extremely low levels of glucose) Branches From Exaggerated Insulin And/Or Serum IGF-1 Levels
Because serum IGF-1 is very similar to insulin, it can produce the same effects as insulin by binding to the cell receptors.[50] Based on my story, I was double counting the production of insulin- one through serum IGF-1 and the other through insulin. The overproduction of insulin eventually lead to hypoglycemia[50], which progressively forced my cell receptors to block the invasion of more insulin from entering into the blood.
Overtime, this vicious cycle lead to a pile up of more sugar in my blood causing some form of insulin resistance (click here to learn more about insulin resistance). We all know insulin resistance is one of the primary causes of hormonal imbalance and hair loss, and sadly, I was most likely the beneficiary.
Take Home Message
What are the key take home lessons we can learn from my story and subject matter?
- First, NEVER, EVER overdo anything! Every body type is different. Some can tolerate more protein than others. High protein diets happen to be the misfortune for my build.
- Second, an overabundance of unbound/free serum (blood) insulin is dangerous to our hair and health because 1) It’s not bound to a pro-hair binding protein – IGFBP-3 -; 2) It spikes the occurrence of type 2 diabetes and cancer 3) It raises estrogen (Hyperestrogenemia); 4) It leads to insulin resistance (hypoglycemia).
- Third, the Western pro-inflammatory diet, too much whey protein, processed meats, and dairy are the major influencers for amplifying free serum insulin.
- Fourth, contrary to serum IGF-1, tissue scalp IGF-1 actually promotes hair growth.
- Fifth, high protein diets, especially in the form of protein powders (whey, soy, etc.) decimates the liver and thyroid and escalates androgenic activity via an uprising of serum IGF-1.
- Sixth, keeping the liver healthy free from radicals, toxins, artificial sugar, refined carbohydrates, and processed foods is the surest way to balance the hormonal scale. Just remember, if the liver is upset, so will your thyroid be!
You can see how hair loss is a symptom of a chain of events that trace back to calm hormone regulation induced by the liver and thyroid. Those two organs are the most important building blocks to repair a crippled mitochondria when the body is in a state of emergency. That state of emergency is “violent” hormonal swings, insulin resistance, and chronic inflammation (by-product of hormonal disturbances).



References
Note: If any blue hyperlinks are broken, you’re NOT out of luck. For your convenience, I have included the origin of these references below in case you want to chase down the full studies.
1. Schmidt JB. Hormonal basis of male and female androgenic alopecia: clinical relevance. Skin Pharmacol. 1994;7(1-2):61-6. doi:10.1159/000211275.
2. Hu H, Zhang S, Lei X, et al. Estrogen Leads to Reversible Hair Cycle Retardation through Inducing Premature Catagen and Maintaining Telogen. Lobaccaro J-MA, ed. PLoS ONE. 2012;7(7):e40124. doi:10.1371/journal.pone.0040124.
3. Montagna W, Ellis RA. The Biology of Hair Growth. New York: Academic Press, 1958: 346. Retrieved from https://books.google.com.
4. Bang HJ, Yang YJ, Lho DS, Lee WY, Sim WY, Chung BC. Comparative studies on level of androgens in hair and plasma with premature male-pattern baldness. Journal of Dermatological Science. 2004;34(1):11-16. doi:10.1016/j.jdermsci.2003.11.005.
5. Berg, E. [Dr. Eric Berg DC]. (2017, April 23). Hormonal Hair Loss [Video File]. Retrieved from https://www.youtube.com/watchtime_continue=4&v=M1zphh8YzD8.
6. Lynfield, YL. Effect of pregnancy on the human hair cycle. Journal of Investigative Dermatology. 1960;35:323-7. doi:10.1038/jid.1960.127.
7. Riedel-Baima B, Riedel A. Female pattern hair loss may be triggered by low oestrogen to androgen ratio. Endocrine Regulations. 2008;42(1):13-16.
8. Conrad F, Ohnemus U, Bodo E, Bettermann A, Paus R. Estrogens and human scalp hair growth-still more questions than answers. Journal of Investigative Dermatology. 2004;122(3):840-842. doi:10.1111/j.0022-202X.2004.22344.x.
9. Kodjo (2012, August 8). Female Pattern Baldness: Menopause, Hair Loss, and Too Much Estrogen. Retrieved from http://kodjoworkout.com/2012/08/menopause-hair-loss-and-too-much-estrogen/.
10. Miller JA, Darley CR, Karkavitsas K, Kirby JD, and Munro, DD. Low sex-hormone binding globulin levels in young women with diffuse hair loss. British Journal of Dermatology. 1982;106(3): 331–336. doi:10.1111/j.1365-2133.1982.tb01732.x.
11. Narad S, Pande S, Gupta M, Chari S. Hormonal Profile in Indian Men with Premature Androgenetic Alopecia. International Journal of Trichology. 2013;5(2):69-72. doi:10.4103/0974-7753.122961.
12. Haffner SM. Sex hormone-binding protein, hyperinsulinemia, insulin resistance and noninsulin-dependent diabetes. Horm Res. 1996;45(3-5):233-237. doi:10.1159/000184794.
13. Daka B, Rosen T, Jansson PA, Larsson CA, Råstam L, Lindblad U. Low sex hormone-binding globulin is associated with hypertension: a cross-sectional study in a Swedish population. BMC Cardiovascular Disorders. 2013;13:30. doi:10.1186/1471-2261-13-30.
14. Sam S. Obesity and Polycystic Ovary Syndrome. Obesity management. 2007;3(2):69-73. doi:10.1089/obe.2007.0019.
15. Haffner SM, Laakso M, Miettinen H, Mykkänen L, Karhapää P, Rainwater DL. Low levels of sex hormone-binding globulin and testosterone are associated with smaller, denser low density lipoprotein in normoglycemic men. The Journal of Clinical Endocrinology & Metabolism. 1996; 81(10):3697-3701. doi:10.1210/jcem.81.10.8855825.
16. Leproult R, Copinschi G, Buxton O, Van Cauter E. Sleep loss results in an elevation of cortisol levels the next evening. Sleep. 1997;20(10):865-870. doi:10.1093/sleep/20.10.865.
17. Spiegel K, Leproult R, Van Cauter E. Impact of sleep debt on metabolic and endocrine function. The Lancet. 1999;354(9188):1435-1439. doi:10.1016/S0140-6736(99)01376-8.
18. Chaput JP, Després JP, Bouchard C, Tremblay A. Association of sleep duration with type 2 diabetes and impaired glucose tolerance. Diabetologia. 2007;50(11):2298-2304. doi: 10.1007/s00125-007-0786-x.
19. Dowling JT, Freinkel N, Ingbar SH. THE EFFECT OF ESTROGENS UPON THE PERIPHERAL METABOLISM OF THYROXINE. Journal of Clinical Investigation. 1960;39(7):1119-1130. doi:10.1172/JCI104127.
20. Schmidt JB. Hormonal basis of male and female androgenic alopecia: clinical relevance. Skin Pharmacol. 1994;7(1-2):61-66. doi:10.1159/000211275.
21. Foitzik K, Krause K, Conrad F, Nakamura M, Funk W, Paus R. Human Scalp Hair Follicles Are Both a Target and a Source of Prolactin, which Serves as an Autocrine and/or Paracrine Promoter of Apoptosis-Driven Hair Follicle Regression. The American Journal of Pathology. 2006;168(3):748-756. doi:10.2353/ajpath.2006.050468.
22. Craven AJ, Nixon AJ, Ashby MG, Ormandy CJ, Blazek K, Wilkins RJ, Pearson AJ. Prolactin delays hair regrowth in mice. Journal of Endocrinology. 2006;(2):415-425. doi:10.1677/joe.1.06685.
23. Torre DL, Falorni A. Pharmacological causes of hyperprolactinemia. Therapeutics and Clinical Risk Management. 2007;3(5):929-951.
24. Wiedemann E, Schwartz E, Frantz AG. Acute and chronic estrogen effects upon serum somatomedin activity, growth hormone, and prolactin in man. The Journal of Clinical Endocrinology & Metabolism. 1976;42(5):942-952. doi:10.1210/jcem-42-5-942.
25. Schmidt JB. Hormonal basis of male and female androgenic alopecia: clinical relevance. Skin Pharmacol. 1994;7(1-2):61-66. doi:10.1159/000211275.
26. Berg, E. [Dr. Eric Berg DC]. (2014, April 29). Understanding Insulin Resistance and What You Can Do About It [Video File]. Retrieved from https://www.youtube.com/watch?v=iTjDi2ZO0n8.
27. Haffner SM. Sex hormone-binding protein, hyperinsulinemia, insulin resistance and noninsulin-dependent diabetes. Horm Res. 1996;45(3-5):233-237. doi:10.1159/000184794.
28. Hirsso P, et al. Association of insulin resistance linked diseases and hair loss in elderly men. Finnish population-based study. Cent Eur J Public Health. 2006;14(2):78-81.
29. Starka L, Duskova M, Cermakova I, Vrbiková J, Hill M. Premature androgenic alopecia and insulin resistance. Male equivalent of polycystic ovary syndrome? Endocrine Regulations. 2005; 39(4):127-131.
30. González-González JG, et al. Androgenetic alopecia and insulin resistance in young men. Clinical Endocrinology. 2009;71(4):494-9. doi:10.1111/j.1365-2265.2008.03508.x.
31. Svegliati-Baroni G, et al. Insulin and insulin-like growth factor-1 stimulate proliferation and type I collagen accumulation by human hepatic stellate cells: differential effects on signal transduction pathways. Hepatology. 1999;29(6):1743-1751. doi:10.1002/hep.510290632.
32. Platz EA, Pollak MN, Willett WC, Giovannucci E. Vertex balding, plasma insulin-like growth factor 1, and insulin-like growth factor binding protein 3. Journal of the American Academy of Dermatology. 2000;42(6):1003-1007. doi:10.1067/mjd.2000.103987.
33. Batch JA, Mercuri FA, Werther GA. Identification and localization of insulin-like growth factor-binding protein (IGFBP) messenger RNAs in human hair follicle dermal papilla. Journal of Investigative Dermatology. 1996;106(3):471-475. doi:10.1111/1523-1747.ep12343649.
34. Wraight CJ, Murashita MM, Russo VC, Werther GA. A keratinocyte cell line synthesizes a predominant insulin-like growth factor-binding protein (IGFBP-3) that modulates insulin-like growth factor-I action. Journal of Investigative Dermatology. 1994;103(5):627-631. doi:10.1111/1523-1747.ep12397667.
35. Weger N, Schlake T. Igfbp3 modulates cell proliferation in the hair follicle. Journal of Investigative Dermatology. 2005;125(4):847-849. doi: 10.1111/j.0022-202X.2005.23886.x.
36. Adachi Y, Nojima M, Mori M, et al. Insulin-like growth factor-1, IGF binding protein-3, and the risk of esophageal cancer in a nested case-control study. World Journal of Gastroenterology. 2017;23(19):3488-3495. doi:10.3748/wjg.v23.i19.3488.
37. Li J, Yang Z, Li Z, Gu L, Wang Y, Sung C. Exogenous IGF-1 promotes hair growth by stimulating cell proliferation and down regulating TGF-β1 in C57BL/6 mice in vivo. Growth Hormone & IGF Research. 2014;24(2-3):89-94. doi:10.1016/j.ghir.2014.03.004.
38. Our Approach to Improve Hair Loss by Increasing Hair Growth Factor IGF-1. (n.d.). JHGC Japan Anti-aging Solutions. Retrieved October 1, 2017, from http://www.jhgc.com.sg/theory/igf-1/.
39. Berg, E. [Dr. Eric Berg DC]. (2017, March 1). Understanding IGF-1 (Insulin-Like Growth Factor) in Simple Terms [Video File]. Retrieved from https://www.youtube.com/watch?v=2bjjIPs3Es0.
40. Melnik BC, John SM, Schmitz G. Over-stimulation of insulin/IGF-1 signaling by western diet may promote diseases of civilization: lessons learnt from laron syndrome. Nutrition & Metabolism. 2011;8:41. doi:10.1186/1743-7075-8-41.
41. Phillips GB. Hyperestrogenemia, diet, and disorders of Western societies. The American Journal of Medicine. 1985;78(3):363-366. doi:10.1016/0002-9343(85)90323-7.
42. Pan A, Sun Q, Bernstein AM, et al. Red meat consumption and risk of type 2 diabetes: 3 cohorts of US adults and an updated meta-analysis. The American Journal of Clinical Nutrition. 2011;94(4):1088-1096. doi:10.3945/ajcn.111.018978.
43. Beasley JM, Gunter MJ, LaCroix AZ, et al. “Associations of Serum Insulin-like Growth Factor (IGF-I) and IGFBP-3 Levels Biomarker-Calibrated Protein, Dairy, and Milk Intake in the Women’s Health Initiative.” The British journal of nutrition. 2014;111(5):847-853. doi:10.1017/S00071145 1300319X.
44. Berg, E. [Dr. Eric Berg DC]. (2014, January 29). The Underlying Root Cause(s) of Your Hair Loss [Video File]. Retrieved from https://www.youtube.com/watch?v=tumJRQ01Hmg.
45. Kuoppala, A. (2017, July 13). Protein and Testosterone: Does Dietary Protein Intake Affect Testosterone Production? Retrieved from https://www.anabolicmen.com/protein-testosterone/.
46. Zhu K1, Meng X, Kerr DA, Devine A, Solah V, Binns CW, Prince RL. The effects of a two-year randomized, controlled trial of whey protein supplementation on bone structure, IGF-1, and urinary calcium excretion in older postmenopausal women. Journal of Bone and Mineral Research. 2011;(9):2298-3306. doi: 10.1002/jbmr.429.
47. Schürch MA, Rizzoli R, Slosman D, Vadas L, Vergnaud P, Bonjour JP. Protein supplements increase serum insulin-like growth factor-I levels and attenuate proximal femur bone loss in patients with recent hip fracture. A randomized, double-blind, placebo-controlled trial. Annals of Internal Medicine. 1998;128(10):801-809. doi:10.7326/0003-4819-128-10-199805150-00002.
48. Platz EA, Pollak MN, Willett WC, Giovannucci E. Vertex balding, plasma insulin-like growth factor 1, and insulin-like growth factor binding protein 3. Journal of the American Academy of Dermatology. 2000;42(6):1003-1007. doi:10.1067/mjd.2000.103987.
49. Signorello LB, Wuu J, Hsieh Cc, Tzonou A, Trichopoulos D, Mantzoros CS. Hormones and hair patterning in men: a role for insulin-like growth factor 1? Journal of the American Academy of Dermatology. 1999;40(2 Pt 1):200-3. doi:10.1016/S0190-9622(99)70188-X.
50. Brainum, J. (2010, February 3). IGF-1: Is It the Real Deal? Retrieved from http://www.ironmanmagazine.com/igf-1-is-it-the-real-deal/.